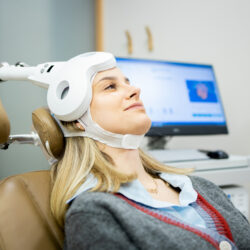
If you’re thinking about transcranial magnetic stimulation for depression, it’s natural to question whether the treatment will be painful.
In short, TMS therapy is usually not painful; most patients experience only mild discomfort or a tapping sensation on the scalp during sessions. For many individuals seeking relief from treatment-resistant depression, understanding what TMS therapy feels like can ease anxiety and help determine if this innovative treatment is right for them.
What Is TMS and What Is It Used to Treat?
Transcranial Magnetic Stimulation (TMS) is a non-invasive procedure that uses magnetic fields to stimulate nerve cells in the brain, primarily to treat major depressive disorder. Unlike surgical methods, TMS requires no anesthesia, incisions, or implanted devices—it is performed entirely on an outpatient basis.
The FDA first approved repetitive TMS (rTMS) in 2008 for adults with major depressive disorder who have not responded to antidepressant medications. Since then, approvals have expanded to include:
Condition | FDA Clearance Year |
|---|---|
Research has also demonstrated promising results for TMS in treating anxiety disorders, post-traumatic stress disorder (PTSD), obsessive-compulsive disorder (OCD), and certain types of chronic pain. Clinical trials continue through 2024-2026 to explore applications for bipolar disorder, generalized anxiety disorder, and other mental health conditions. | |
Treatment-resistant depression | 2008 |
Obsessive compulsive disorder (OCD) | 2018 |
Smoking cessation (adults 22-75) | 2020 |
During TMS treatment, an electromagnetic coil delivers targeted magnetic pulses to brain regions involved in mood regulation (typically the left dorsolateral prefrontal cortex for depression). TMS therapy is usually administered in a series of sessions, typically five times a week for four to six weeks, to achieve the best outcomes. Each session lasts about 20 minutes, during which the coil delivers magnetic pulses to influence brain activity
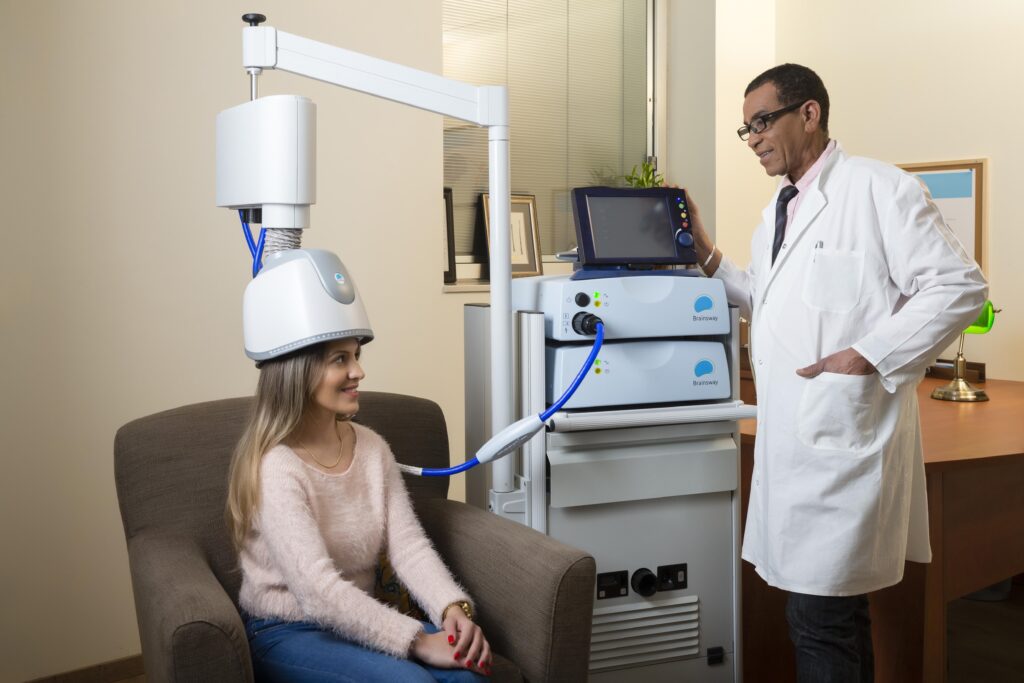
Does TMS Hurt? What It Actually Feels Like
TMS generally does not cause deep or persistent pain. Many patients experience mild discomfort during early sessions, but these sensations are superficial and localized.
The most common feeling during TMS is a rapid, rhythmic tapping on the scalp, often described as similar to a fingertip tapping or a woodpecker pecking. Most patients feel sensations confined to the scalp area where the magnetic coil is placed, which stop during pauses in the pulses.
Patients commonly report:
- Tapping sensation: Rhythmic knocking or prickling on the scalp
- Mild tingling: Comparable to holding a vibrating device against the skin
- Facial muscle twitching: Brief twitches in the forehead, jaw, or eyelids during pulses
Most patients find TMS tolerable and do not describe the experience as painful, according to Harvard Health. While some find the sensations slightly uncomfortable, most can read, listen to music, or converse with staff during treatment.
Discomfort often decreases as patients become accustomed to the magnetic pulses, with many noting the sensations become less noticeable after several sessions. If the tapping feels sharp or unbearable, inform your technician immediately. They can adjust the intensity and coil position.
Common Side Effects of TMS
TMS is generally well tolerated, with side effects typically mild and short-lived. Most patients experience side effects during or shortly after treatment sessions.
Common side effects of Transcranial Magnetic Stimulation (TMS) include mild headaches and scalp discomfort, which typically resolve within a few hours after treatment sessions.
Short-Term Side Effects
Other short-term side effects include:
- Facial or eyelid muscle twitching during pulses
- Brief jaw, tooth, or ear discomfort
- Temporary lightheadedness or fatigue
Muscle twitching during TMS occurs because magnetic fields stimulate nearby motor nerves in the face, jaw, or scalp. These effects result from nerve and muscle stimulation in the scalp area, not from any damage to brain tissue or activity.
TMS produces a loud clicking sound similar to a metronome, so patients usually wear earplugs during treatment. This hearing protection is standard and recommended for every session.
Serious Risks Are Extremely Rare
Serious risks, such as seizures, are extremely rare, occurring in fewer than 0.1% of patients during TMS sessions (according to research published in Brain Stimulation). Still, to be on the safe side, you are screened for risk factors such as metal implants, aneurysm clips, cochlear implants, and seizure history before starting treatment.
Early Mood Changes Are Temporary
Some patients may experience temporary intensification of depression or anxiety symptoms at the beginning of TMS treatment, which usually subsides as treatment progresses.
How Long Do TMS Side Effects and Discomfort Last?
Most side effects begin during treatment and fade within minutes to a few hours afterward. Mild headaches and scalp discomfort typically resolve within a few hours after treatment sessions.
As patients continue treatment, side effect intensity usually decreases as they become accustomed to the coil delivering magnetic pulses. Many report minimal discomfort by weeks 3-4 of a typical 6-week course.
Muscle twitches and unusual sensations cease immediately when the machine is turned off. There is no lingering effect. The procedure is non-invasive, allowing patients to resume normal activities, including driving, immediately after sessions.
Any side effect lasting more than a day or interfering with daily life should be reported to your clinician.
What to Expect During a TMS Session
Knowing what to expect during TMS can ease anxiety and reduce discomfort:
First Appointment:
- Medical review and safety screening for seizure history or metal implants
- Motor threshold mapping to determine the lowest intensity that causes a thumb twitch
- Mapping may feel slightly more intense as the technician finds the correct spot
Routine Treatment Sessions:
- You sit comfortably in a comfy chair
- Some patients wear ear protection (earplugs or headphones)
- A helmet is placed on top of your head
- Treatment starts with brief trains of pulses (seconds on, seconds off)
During stimulation, you’ll hear rapid clicking and feel tapping on your scalp. Pulses come in short bursts with breaks to prevent fatigue.
You remain awake and alert throughout. You can pause the session by raising a hand and leave immediately afterward without restrictions. Many patients read, watch TV, or relax during sessions.

What Should You Do If TMS Feels Uncomfortable?
If you experience discomfort during TMS, speak up early, especially during initial sessions. Our care team can make real-time adjustments to improve comfort.
Clinical adjustments include:
- Lowering stimulation intensity below standard levels
- Gradually increasing intensity over 3-5 sessions
- Repositioning the coil to avoid sensitive nerves
- Adding thin foam padding beneath the coil
Comfort strategies:
- Taking over-the-counter pain relievers 30-60 minutes before sessions if headaches are frequent
- Arriving well-hydrated and having a light snack before treatment
- Managing caffeine intake, as caffeine can lower motor threshold
- Practicing relaxation or breathing exercises during treatment
- Bringing a friend or family member along for extra support
- Wearing earplugs (which we provide at every session)
- Using a mouth guard (offered free of charge across all our clinics)
- Chatting with your technician — our team is always there and happy to talk
Relaxation techniques can meaningfully reduce discomfort. If sensations remain severe despite adjustments, we may consider alternative coil types, protocol changes such as theta-burst stimulation, or pausing treatment.
Is TMS More or Less Painful Than Other Depression Treatments?
Compared to other depression treatments, TMS is among the more comfortable options.
Treatment | Pain/Discomfort Level | Key Considerations |
|---|---|---|
TMS | Mild scalp tapping | No anesthesia, immediate return to activities |
Electroconvulsive therapy (ECT) | Requires anesthesia | May cause muscle soreness, possible memory loss, needs anesthesia, you can’t drive yourself home, it’s invasive |
Antidepressant medications | No scalp pain | Systemic effects: weight changes, sexual dysfunction, GI upset, lower success rates |
Deep brain stimulation | Surgical procedure | Incisions, implants, infection risk |
TMS offers a middle ground: brief, localized sensations during sessions with minimal systemic side effects and no cognitive impairment. For many, this balance makes TMS an appealing depression treatment.
Patients often notice improvements in mood, energy, and functioning as therapy takes effect, with some seeing significant benefits after just a few sessions.
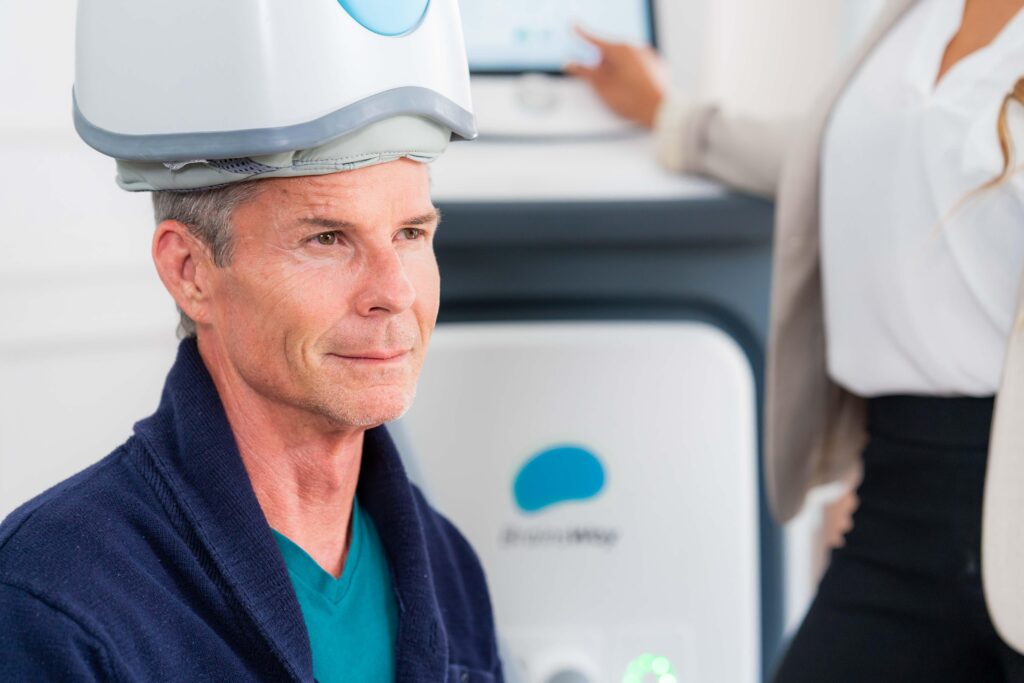
Ready to Find Out If TMS Is Right for You?
Wondering whether TMS will hurt is one of the most natural questions to ask, and now you have your answer. For most people, a little scalp tapping and the sound of clicking is all that stands between them and a treatment that could change their life.
At Oasis Mental Health Centers in New Jersey, we walk every patient through exactly what to expect before their first session so there are no surprises. If you’re ready to take the next step toward lasting relief from depression, reach out to us today and let’s find out if TMS is the right fit for you.
FAQs
Is TMS safe if I have migraines or a low pain tolerance?
Many patients with migraine histories complete TMS successfully, though they may feel scalp discomfort and noise more intensely. You’ll want to share your migraine history and medications with us first so treatment intensity and schedule can be tailored to your needs.
A low pain threshold isn’t a disqualifier. Gradual dose increases and open communication help keep treatment manageable.
Will I feel anything in my brain or have memory problems from TMS?
Sensations occur on the scalp and superficial facial muscles, not inside the brain. The brain itself lacks pain receptors like the skin.
Unlike ECT, standard rTMS has not been shown to cause memory loss or confusion. Many patients report clearer thinking as depression improves. Any new cognitive issues should be discussed with your clinician.
Does deep TMS or theta burst stimulation hurt more than standard rTMS?
Deep TMS (the technology we use at Oasis through BrainsWay) uses a specialized H-coil helmet to reach broader brain areas and may produce a more diffuse pressure sensation, but it remains well tolerated.
Intermittent theta burst stimulation (iTBS) delivers pulses in rapid bursts, shortening sessions to 3-10 minutes. Some patients find this easier to tolerate. However, comfort depends more on individual sensitivity and coil placement than protocol type, and adjustments can always be made.
How do I know if I’m a good candidate for TMS despite concerns about pain?
Schedule an evaluation with us and we’ll review your psychiatric history, past treatments, and any contraindications like metal implants. You’ll have the chance to handle the coil, hear the machine, and ask us anything.
If you meet the safety criteria, most people concerned about pain can move forward with confidence. We’ll customize your treatment plan and gradually increase intensity over your initial sessions so you’re always comfortable. TMS mainly treats major depressive disorder (MDD), especially for patients who haven’t found relief from medications and psychotherapy.
We believe that for many people, a few weeks of mild discomfort is worth the chance of lasting relief.